ROOT CANALS
Treat the pain of infected teeth!
A root canal is a treatment used to repair and save a tooth that is badly decayed or becomes infected.
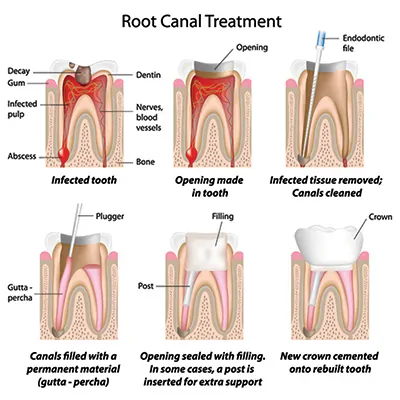
During a root canal procedure, the nerve and pulp are removed and the inside of the tooth is cleaned and sealed.
Without treatment, the tissue surrounding the tooth will become infected and abscesses may form. “Root canal” is the term used to describe the natural cavity within the center of the tooth. The pulp or pulp chamber is the soft area within the root canal. The tooth’s nerve lies within the root canal. A tooth’s nerve is not vitally important to a tooth’s health and function after the tooth has emerged through the gums. Its only function is sensory — to provide the sensation of hot or cold. The presence or absence of a nerve will not affect the day-to-day functioning of the tooth.
Process for a root canal
What to expect after your root canal
For the first few days following the completion of a root canal, the tooth may feel sensitive due to natural tissue inflammation, especially if there was pain or infection before the procedure. This sensitivity or discomfort usually can be controlled with over-the-counter pain medications such as ibuprofen (Advil, Motrin) or naproxen (Aleve). Most patients can return to their normal activities the next day.
Until your root canal procedure is completely finished — that is to say, the permanent filling is in place and/or the crown, it’s wise to minimize chewing on the tooth under repair. This step will help avoid re-contamination of the interior of the tooth and also may prevent a fragile tooth from breaking before the tooth can be fully restored. As far as oral health care is concerned, brush, floss, and use an antiseptic mouthwash as you regularly would and see your dentist at normally scheduled intervals.
Call us now for a pain-free Root Canal experience!
If you have questions about root canal treatments or need to schedule an appointment, contact Maple Dental at 760-949-7274. Our caring team is here to ensure your comfort and provide the highest quality dental care for a healthy smile. Don’t hesitate to reach out today!



